More Info
A healthcare worker collects a sample from a man in his car at a COVID-19 mobile testing unit.
JHDT Productions / Shutterstock
Understanding COVID-19 data: Age isn’t everything
This piece is part of a series, presented by our partner SAS, that explores the role of data in understanding the COVID-19 pandemic. SAS is a pioneer in the data management and analytics field. (Check out other posts in the series on our Get Smart About COVID-19 Misinformation page.)
As the United States enters its seventh month in the grip of the COVID-19 pandemic, we have seen myths created and debunked, fears and hopes elevated and dashed, and initial assumptions become lessons learned.
The most important piece of conventional wisdom proven false is that the virus targeted only older people and that younger generations were largely safe from infection. However, data released by the Centers for Disease Control and Prevention (CDC) on June 19 tells a different story. As of May 30, 70% of those who tested positive for COVID-19 were under 60. In March, by comparison, approximately 25% of positive cases occurred in people under 50.
One theory for the surge of cases in those under 60 is that in the early days COVID-19 testing was restricted to only the sickest patients. Therefore, many people with mild cases — often those under age 65 — may not have been diagnosed. Regardless, the new CDC report underscores that younger generations are vulnerable to COVID-19 infections and can get very sick or die.
Yet, the elderly and those with certain chronic health conditions do remain most vulnerable to severe illness and death. Experts have been exploring questions about vulnerability and how to protect at-risk populations since an outbreak of 129 cases of COVID-19 among patients, staff and visitors resulted in 40 deaths at a Kirkland, Washington, nursing home in February.
COVID-19 risk factors about more than age
Initially, public health officials focused primarily on age when evaluating COVID-19 vulnerability. But the definition of vulnerability quickly expanded to include those with underlying health conditions like diabetes, asthma, cardiovascular disease, and obesity. We now know that individuals over age 65 who contract COVID-19 are more likely to develop severe complications not solely due to age, but also because they may also have underlying health conditions. This partly explains why 40% of U.S. deaths from COVID-19 have occurred in nursing homes and other long-term care facilities.
Knowing that age and underlying health conditions help determine the risk of vulnerability is important, but it doesn’t fully explain why so many cases occur in those facilities.
Other factors that aid in the spread of infectious disease may be present:
- Shortages of personal protective equipment like masks and gowns can hinder necessary precautions.
- Shared bedrooms and common living spaces among residents make it nearly impossible to effectively socially distance.
- Transfers of residents from hospitals and other locations can introduce exposure to disease.
- Frequent visitors, employees and other providers coming from outside the facility further increase risk.
Data makes the difference
Analyzing data about aging populations helps us better understand why these individuals are at greater risk for COVID-19. For example, we can use data to see where the most vulnerable populations are located and how they are impacted by the virus. When we look at the geographic distribution of population by age along with data on secondary conditions that may be present, we get a better idea of the dangers facing aging populations. This deeper knowledge reveals how contributing factors can lead to high susceptibility to COVID-19 and helps us understand how to protect these populations
There are more than 50 million Americans over the age of 65. California, Florida, Texas and New York have the highest number of older Americans, with Sumter County, Florida, having the highest overall percentage in the nation.
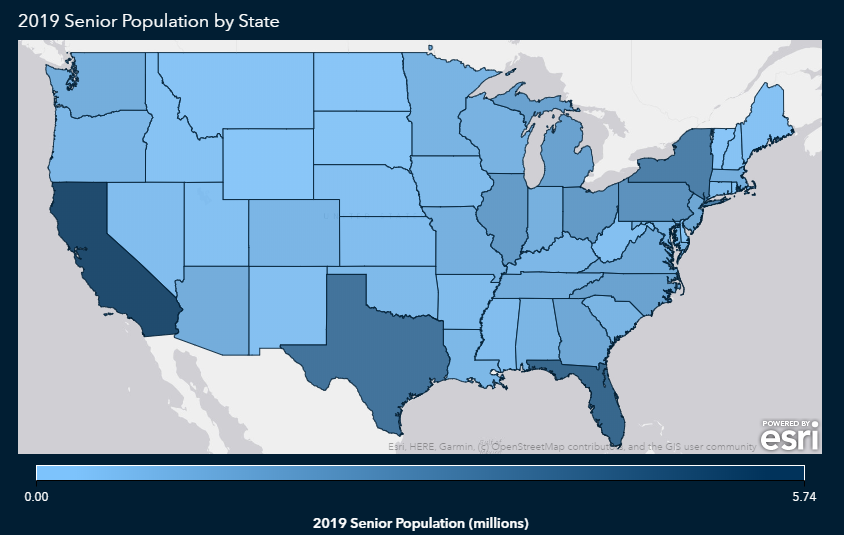
As we might expect, those states also have higher concentrations of people over age 85, since that’s a subset of the 65-and-over population.
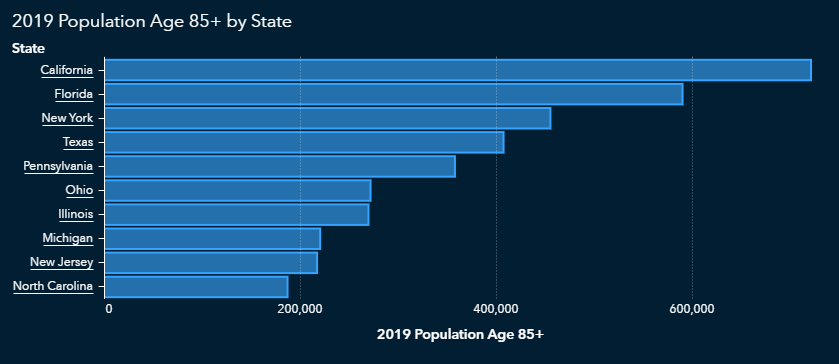
Do COVID-19 risk factors follow state lines?
Obesity and diabetes often go together, and according to CDC data, the states most affected by obesity and diabetes overlap and tend to be concentrated in the southern United States.
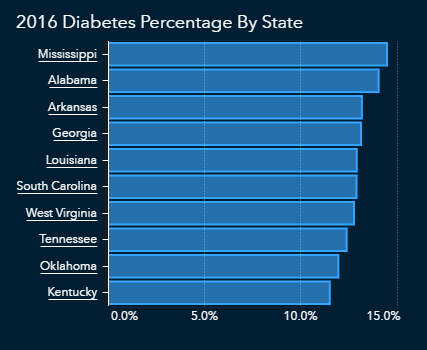
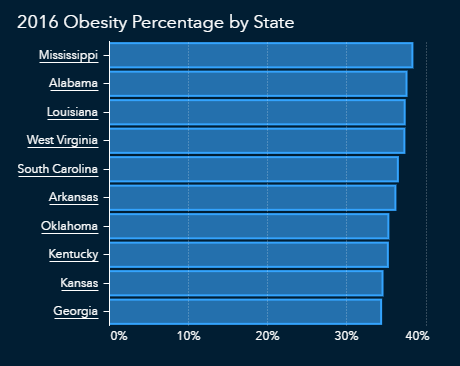
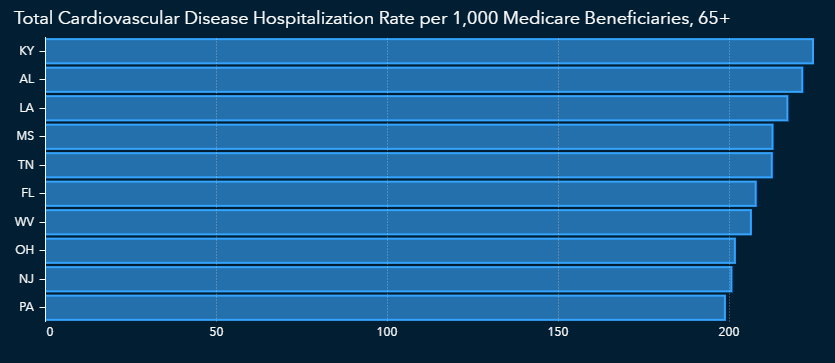
The CDC also reports cardiovascular disease in terms of hospitalizations, with a focus on those over age 65. The data shows an overlap with states that have higher numbers of diabetes and obesity. This could mean that those hospitalized with cardiovascular disease might also have diabetes and/or obesity, which would put them at even higher risk of severe complications from COVID-19.
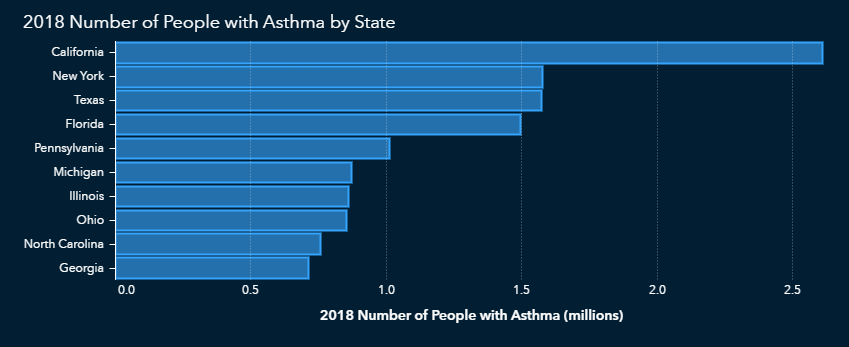
Finally, we must look at data regarding lung conditions such as asthma. Some states with a high incidence of asthma cases overlap with those states that have large populations with at least one of the other risk factors we’ve examined.
What does all this mean?
The data appears to show that there are vulnerable people everywhere in the U.S., but there are concentrations in several areas. As states loosen restrictions initially put in place when the pandemic hit the U.S., it becomes important to evaluate population data within each state to ensure that those who are most vulnerable are protected. In recent weeks we have seen upticks in cases in some states that loosened restrictions.
It is crucial that we identify risk factors and set up proper safeguards. By evaluating additional risk factors and analyzing data within our own communities, we gain a more complete understanding of the COVID-19 impact. When we consider the whole individual, rather than age alone, we better understand what it means to be vulnerable during this pandemic and going forward.
Other articles in this series:
![]() About SAS: Through innovative analytics software and services, SAS helps customers around the world transform data into intelligence.
About SAS: Through innovative analytics software and services, SAS helps customers around the world transform data into intelligence.